The ongoing flu season in the United States is currently being described as particularly severe and intense, demonstrating hospitalization rates that occasionally surpass those seen during the height of the Covid-19 pandemic. At some points in recent months, the hospitalization figures have been alarming—as reported by healthcare officials, a significant number of patients are facing severe complications triggered by flu infections.
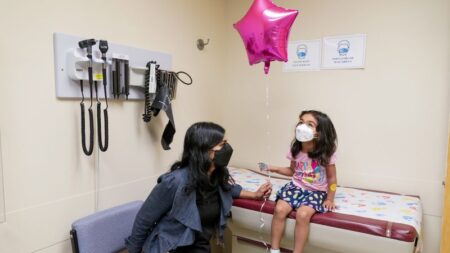
Among children, an unusual trend has emerged with an uptick in hospital admissions due to neurologic complications, one of the most concerning being acute necrotizing encephalopathy (ANE). This disturbing condition, characterized by severe brain swelling leading to tissue death, has captured the attention of pediatric specialists who are increasingly witnessing its occurrence in their clinics. Dr. John Lynch from UW Medicine has noted a related danger in adults: an unexpected prevalence of necrotizing pneumonia caused by methicillin-resistant Staphylococcus aureus (MRSA), a particularly virulent superbug that resists many traditional antibiotics.
Dr. Lynch remarked that many patients exhibit indications of severe lung damage following influenza, which is concerning given that such bacterial pneumonia infections often descend upon individuals recovering from the flu—especially older adults. The high volume of hospitalizations has also forced healthcare professionals across the country, including critical care nurses who document their experiences on platforms like Reddit, to express their concerns about the alarming rise in flu-related illness.
Nationally, as of the week ending February 1, flu hospitalization rates have reached 14.4 for every 100,000 people, which is slightly elevated compared to Covid-19 hospitalizations during the Delta wave’s peak in September 2021. Moreover, the Centers for Disease Control and Prevention (CDC) have noted that the cumulative flu hospitalizations this season are now greater than those for Covid-19—a first since the Covid pandemic began. Figures reveal approximately 64 flu hospitalizations for every 100,000 people, contrasting sharply with the 44 Covid-19 hospitalizations in the same demographic during this season.
Furthermore, flu fatalities have outpaced Covid-related deaths for the first time, with CDC-confirmed deaths showing 1,302 from influenza in the last two weeks of January, eclipsing the 1,066 Covid fatalities. Across the nation, the flu activity reported by the CDC indicates robust transmission, with about one-third of flu tests returning positive results. In some regions, positivity rates have risen as high as 50%, particularly in areas like Washington, where Dr. Lynch practices.
An exploration into ANE cases has shown that neither pediatricians nor other professionals are mandated to report these instances, complicating efforts to track trends and increases. Evidence from Stanford Medicine indicates a troubling rise in severe flu cases leading to neurological complications among children. It is hypothesized that the flu, among other viral infections, may invoke ANE, which can be fatal in conjunction with brain swelling, especially in the critical area of the thalamus—responsible for regulating sleep and wakefulness.
The current flu strain landscape comprises two strains of influenza A—H1N1 and H3N2—each significantly active, with epidemiologists observing unusual equal prevalence rates rather than the typical predominance of a single strain. Compounding this issue is the low vaccination coverage, which has dropped considerably among both adults and children compared to pre-pandemic levels, raising concerns amongst health professionals about the potential for adverse outcomes this season.
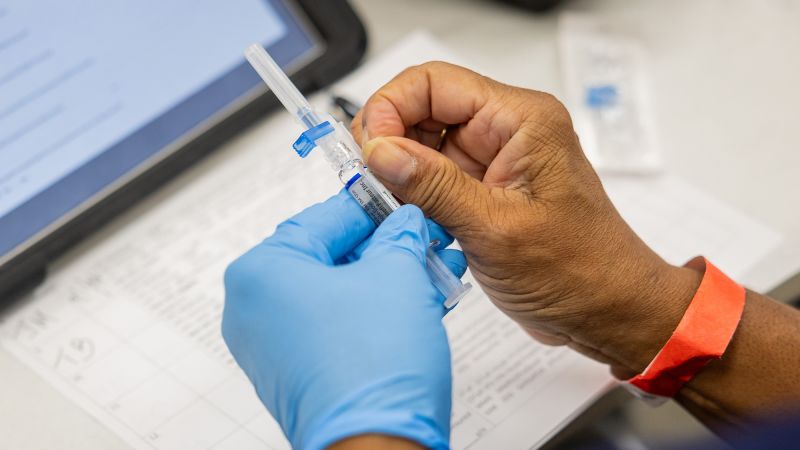
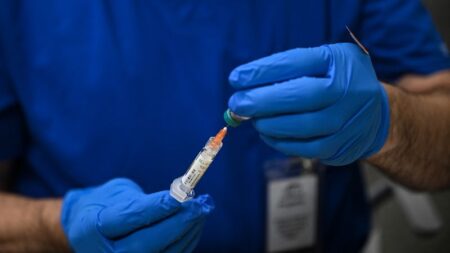
Amidst these alarming statistics, the medical community emphasizes the importance of getting vaccinated, practicing good hygiene, and managing exposure risks to mitigate severe flu cases. Even with the flu vaccine, breakthrough infections can occur; however, vaccinations can lead to less severe illness. The experts implore individuals to engage in preventive measures as the flu season continues, asserting that the situation demands heightened public awareness and a concerted effort to reduce the health impacts across various communities.
In these challenging times, healthcare providers invite the public to remain proactive and utilize available vaccines, maintain good hygiene practices, and if needed, use antiviral medications early in the course of infection to avoid severe consequences. As we navigate this severe flu season, the collaboration of healthcare professionals and public health initiatives becomes increasingly vital to safeguarding public health effectively.