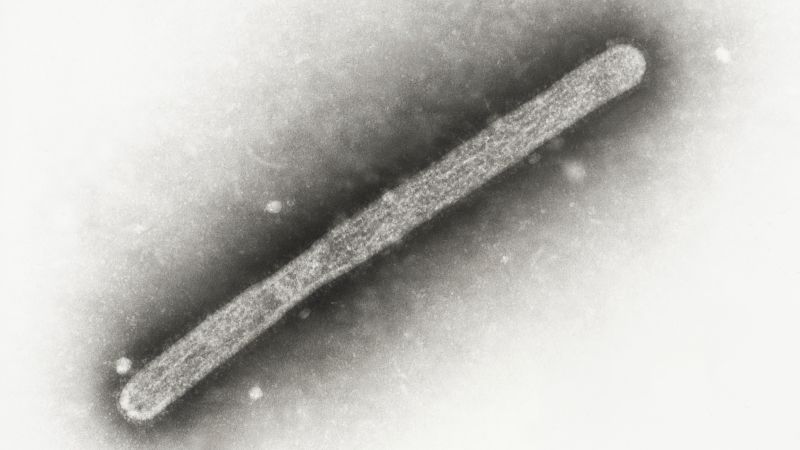
In a significant public health event, the Louisiana Department of Health has confirmed the death of the first person in the United States who had a severe case of H5N1 bird flu. This unfortunate event marks the first human fatality due to bird flu in the country, igniting concerns within medical communities and among public health officials. The emergence of this case reflects ongoing global vigilance as avian influenza continues to pose risks to both animal and human populations.
The individual who succumbed to the virus was reported to be over the age of 65 and had pre-existing medical conditions that likely contributed to the severity of the illness. Prior to hospitalization, the individual had been exposed to a backyard flock of birds, as well as wild birds, which are often environments where the virus can be contracted. Given the nature of H5N1 and its effects on individuals, especially those with underlying health issues, this tragic instance underscores the importance of awareness and caution when engaging with birds, whether domesticated or wild.
Following the investigation by Louisiana health officials, there was reassuring news that no other human cases had been directly linked to this individual’s infection. This suggests that the virus has not spread in a manner that poses an immediate broader public health threat. Nonetheless, the monitoring and investigation of such cases continue to remain a priority, as the situation evolves.
The specific clade of the bird flu virus that infected the patient has been identified as D1.1. This strain is currently circulating in both wild birds and poultry, differing from other variants that may be present in livestock such as dairy cattle. The Centers for Disease Control and Prevention (CDC) conducted a genetic analysis of the virus in late December. Their findings indicated changes in the virus’ genetic structure that could enhance its ability to infect the upper airways of humans and increase its potential for human-to-human transmission. Importantly, these genetic changes were not detected in the avian populations the infected individual had been exposed to, suggesting that adaptations may have occurred after human infection.
Despite this alarming information, health authorities have reiterated that the overall risk to the general public remains low. However, individuals who maintain backyard chickens or other birds, as well as employees working on poultry and dairy farms, are considered to be at a relatively higher risk for potential infection. Recommendations have been issued for those who work with animals—urging them to remain vigilant for symptoms such as respiratory difficulties and conjunctivitis, particularly within a 10-day timeframe following any potential exposure. A timely report to healthcare providers regarding such exposures is also advised.
To mitigate risks and promote safety, a variety of protocols have been proposed. First and foremost, it is crucial for individuals to avoid touching sick or dead birds or their droppings. Furthermore, pet owners should ensure that their animals are kept away from these potentially infected creatures. Food safety practices are equally important; consuming fully cooked poultry and eggs and avoiding raw or undercooked products can significantly reduce the risk of transmission. For those employed on farms, consulting with healthcare professionals about seasonal flu vaccinations is another recommended strategy to minimize the possibility of co-infection.
Moreover, it is essential to report any sightings of sick or deceased birds or livestock to the U.S. Department of Agriculture. This facilitates appropriate action and enhances efforts to monitor and control the spread of avian influenza.
This article reflects an evolving story as public health officials continue to gather information and provide updates regarding this incident and its implications. The situation serves as a stark reminder of the ongoing need for vigilance in dealing with zoonotic diseases and the potential impact of wildlife interactions on human health.